홈 > 연구소 > 논문 / 학술활동
연구소
마마파파&베이비의 핵심인 베이비 드림 난임 연구소는
그간의 연구학술 성과에 안주하지 않고,
늘 한계를 뛰어넘기 위해 노력합니다.
정액처리 배양액에 Myoinositol의 첨가는 무력정자증 환자의 인공수정시술 시 정자의 운동성과 임신율을 향상시켰다.
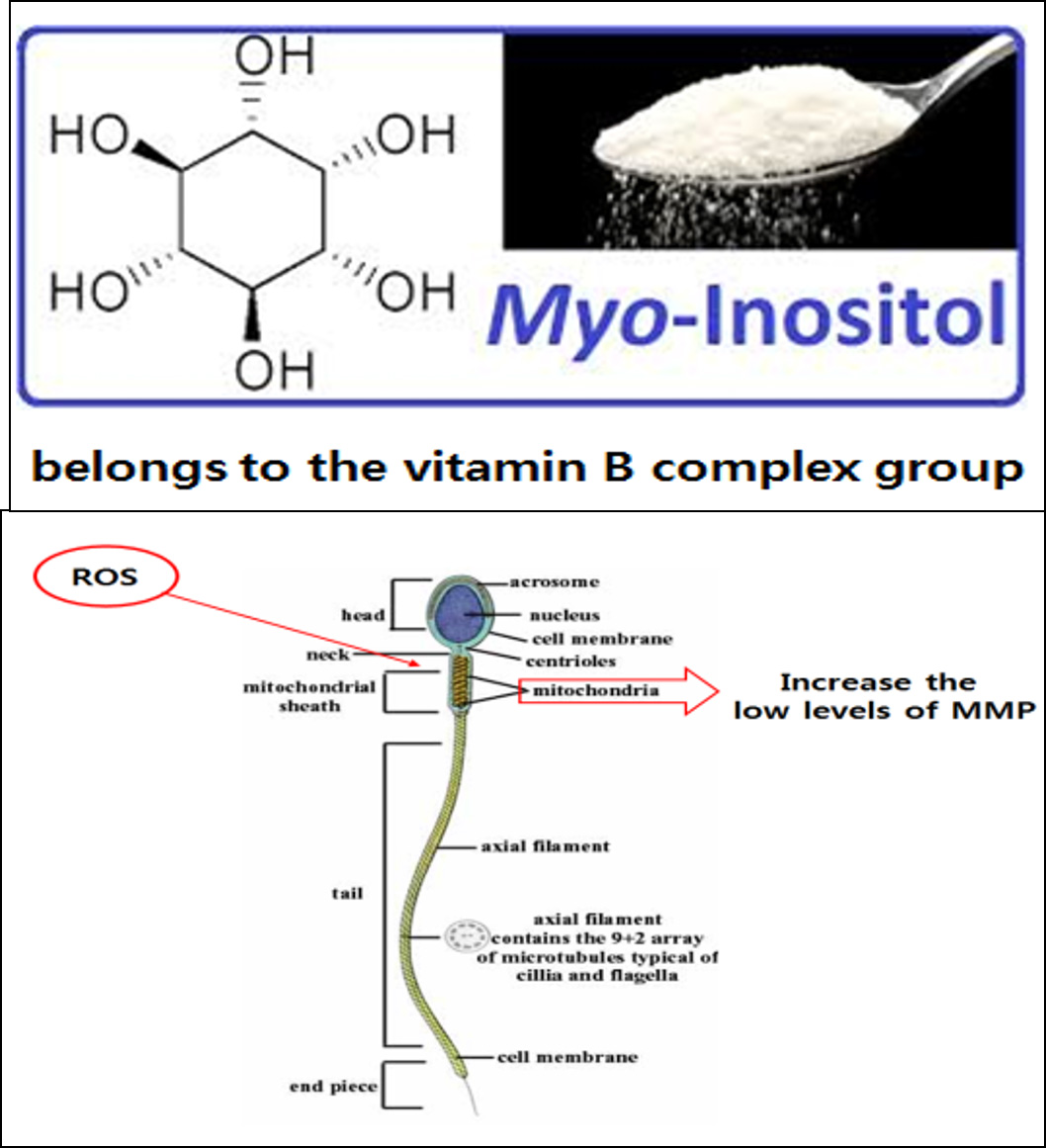
2016년 유럽불임학회(ESHRE) P-022 Addition of myoinositol into sperm preparation medium improved the sperm motility and pregnancy rate of IUI cycles in asthenozoospermic patients. (정액처리 배양액에 Myoinositol의 첨가는 무력정자증 환자의 인공수정시술 시 정자의 운동성과 임신율을 향상시켰다.)
Park, JY.(1)*;Kim, SG.(1);Kim, YY.(1);Kwak, SJ.(1);Yoo, CS.(1);Lee, KH.(1);Park, IH.(1);Sun, HG.(1);Cho, JD.(1);Chi,HJ.(1);
(1)Infertility center, Mamapapa&baby Ob/Gy Clinic, Ulsan, Korea- South;
(2)Infertility center, Elle-Medi Clinic., Changwon, Korea- South
Study question
This study was performed to evaluate the effects of myoinositol (MI) on sperm motility and clinical outcomes of IUI cycles.
Summary answer
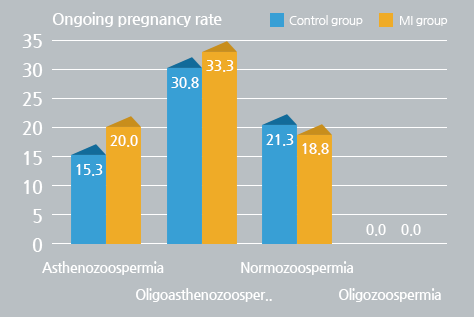
Myoinositol improved the sperm motility and pregnancy rate of IUI cycles in asthenozoospermic patients, but it didn’t show any beneficial effect in normozoospermic patients.
What is known already
Percentage of spermatozoa with high mitochondrial membrane potential (MMP) levels showed a correlation with high fertilization rate because the MMP level of sperm is directly associated with motility of sperm. However the MMP level is inversely correlated with ROS level that induce a damage to the mitochondrial membrane. MI increased the percentage of spermatozoa with high MMP level in the patients with abnormal sperm parameters. Moreover, MI increased fertilization and pregnancy rates in women who failed to pregnancy due to poor oocyte quality by reducing oxidative stress in culture conditions.
Study design, size, duration
A prospective study was carried out to investigate the effects of MI on sperm motility and clinical outcomes in IUI cycles from August to December 2015. Total 376 patients (IUI cycles) were divided into two groups according to the addition of MI into sperm preparation medium; MI group (n=144) and Control group (n=232). Both groups were subdivided into 3 groups according to the result of semen analysis; Normozoo-, Asthenozoo-, and Oligoasthenozoo-spermic patient groups.
Participants/materials, setting, methods
Raw semen was treated with density gradient centrifugation for isolation of motile sperm, and then the motile sperm was washed twice with Ham’s F-10 with or without 5mg/ml MI. An antioxidant effect of MI on the sperm motility suppressed by hydrogen peroxide was investigated to identify the enhancing effect of MI on motility.
Main results and the role of chance
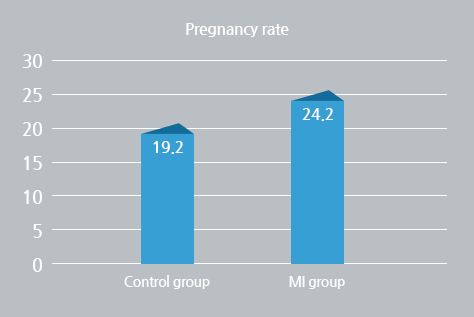
The effects of various MI concentrations (0, 2, 5, 10, 20 mg/ml) on motility of raw semen was investigated. Even the treatment with low concentration of 5mg/ml significantly increased the motility (38.1%) compared to the treatment without MI (21.5%, P<0.01). Unlike the raw semen, however, in the motile sperm isolated by density gradient centrifugation, the sperm motility in the MI group was not different from the motility in the control group (87.1% vs 83.5%). Between the MI and Control groups, there were no differences in the age of patients (female; 33.7 vs. 34.1, male; 35.9 vs.35.9), volume (3.4 vs. 3.3ml), count (89.5 vs. 101.8x106/ml), and motility (42.1 vs. 47.3%) of the raw semen. The pregnancy rates of asthenozoo- (28.8%) and oligoasthenozoo-spermic patients (33.3%) in the MI group were higher than those of control group (18.8 and 25.0%, respectively), although a statistical significance was not observed in the difference. Addition of hydrogen peroxide significantly decreased the sperm motility in a concentration-dependent manner. The suppressive effect of hydrogen peroxide was significantly reversed by addition of MI.
Limitations, reason for caution
The limitations of the present study included the limited number of samples tested, which slightly reduced the study’s statistical power.
Wider implications of the findings
MI improved sperm motility and pregnancy rate of IUI cycles in asthenozoospermic patients. The beneficial effect of MI may be associated with antioxidant activity as well as improvement of MMP level. Therefore, MI also may be useful for IVF-ET cycles in asthenozoospermic patients.
-
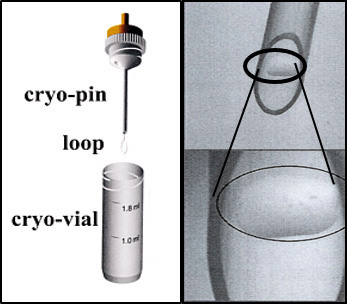 2017년 유럽불임학회(ESHRE) P-
Cryo-loop와 Hemi-straw를 이용한 인간 배아 유리화 동결에서 해동 후 손상되지 않은 배아와 임상 결과의 비교.
2017년 유럽불임학회(ESHRE) P-
Cryo-loop와 Hemi-straw를 이용한 인간 배아 유리화 동결에서 해동 후 손상되지 않은 배아와 임상 결과의 비교.
-
 2016년 미국불임학회(ASRM) P-595
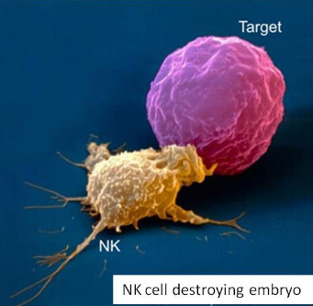
반복착상 실패 환자 에서 면역치료요법이 유용할 것인가; 특히 높은 자연살해세포를 가진 환자에서?
2016년 미국불임학회(ASRM) P-595
반복착상 실패 환자 에서 면역치료요법이 유용할 것인가; 특히 높은 자연살해세포를 가진 환자에서?
-
 2016년 미국불임학회(ASRM) P-555
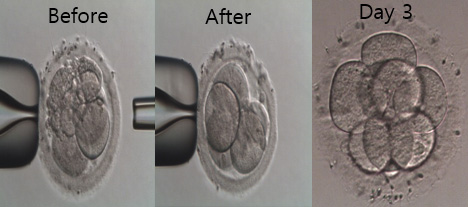
2일 째 파편화된 인간 배아에서 파편제거는 순차적 배아의 발달과 임상적 결과를 유의하게 증가시킨다.
2016년 미국불임학회(ASRM) P-555
2일 째 파편화된 인간 배아에서 파편제거는 순차적 배아의 발달과 임상적 결과를 유의하게 증가시킨다.
-
 2016년 미국불임학회(ASRM) P-317
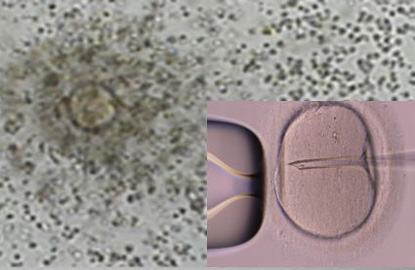
정자 DNA 파편화 지수가 높은 환자에서 ICSI가 전통적인 IVF에 비해 임신율을 유의하게 증가시켰다.
2016년 미국불임학회(ASRM) P-317
정자 DNA 파편화 지수가 높은 환자에서 ICSI가 전통적인 IVF에 비해 임신율을 유의하게 증가시켰다.
-
 2016년 미국불임학회(ASRM) P-263
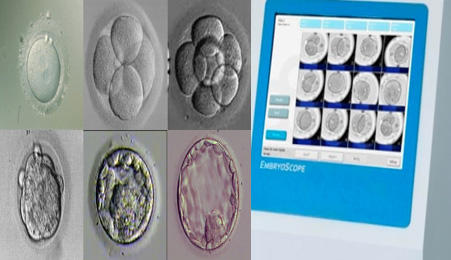
연속 배아 채점 시스템은 Time-lapse 모니터링 시스템 대신 사용할 수 있습니다.
2016년 미국불임학회(ASRM) P-263
연속 배아 채점 시스템은 Time-lapse 모니터링 시스템 대신 사용할 수 있습니다.
-
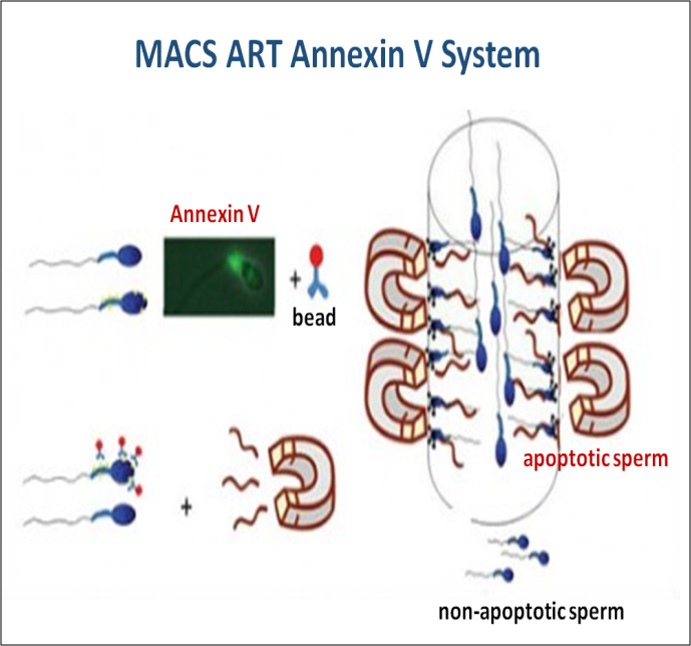 2016년 유럽불임학회(ESHRE) P-021
중층원심분리와 자석활성화세포분리 방법의 병용은 정액샘플의 정자 DNA손상지수를 유의하게 감소시킨다.
2016년 유럽불임학회(ESHRE) P-021
중층원심분리와 자석활성화세포분리 방법의 병용은 정액샘플의 정자 DNA손상지수를 유의하게 감소시킨다.
-
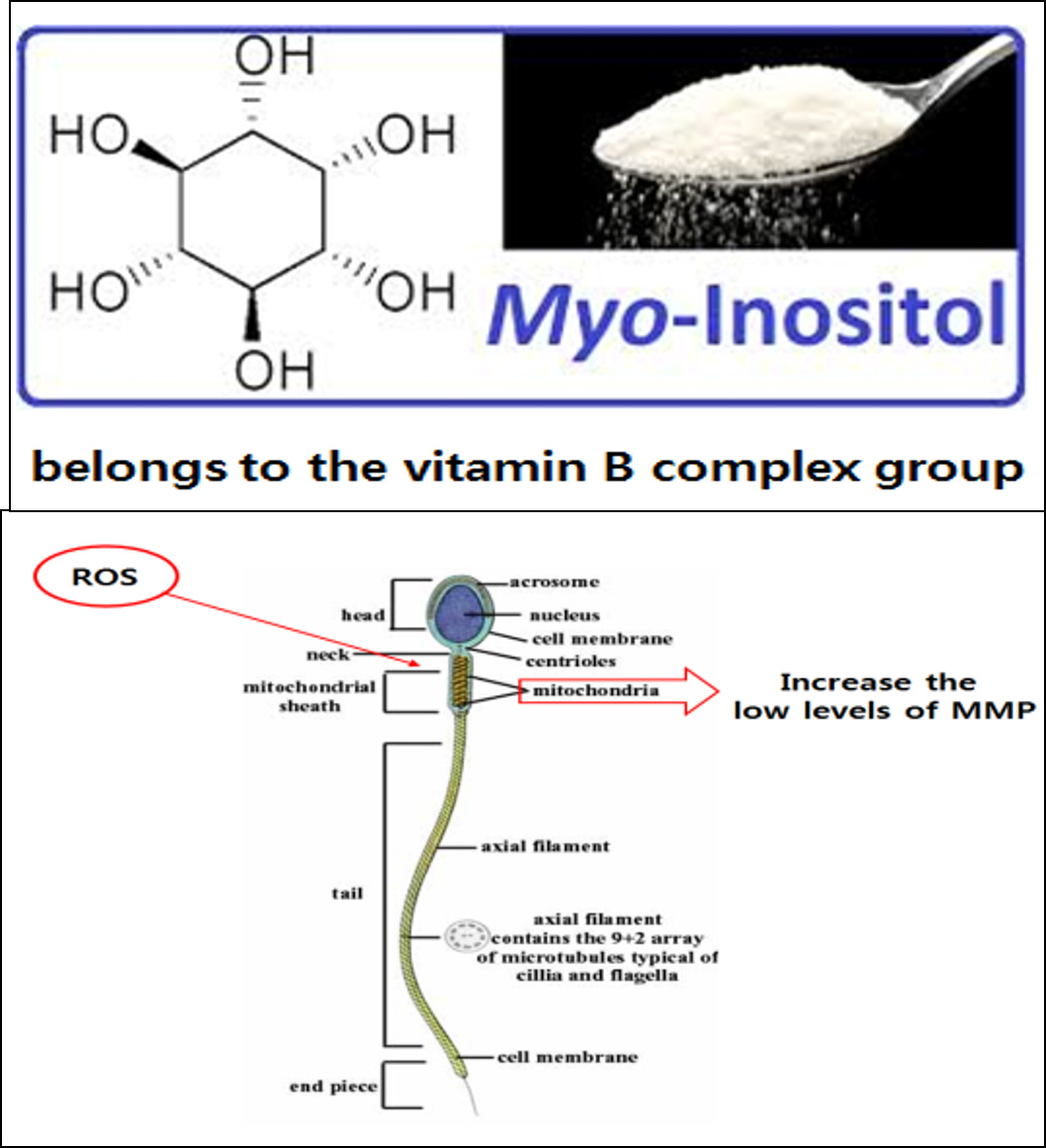 2016년 유럽불임학회(ESHRE) P-022
정액처리 배양액에 Myoinositol의 첨가는 무력정자증 환자의 인공수정시술 시 정자의 운동성과 임신율을 향상시켰다.
2016년 유럽불임학회(ESHRE) P-022
정액처리 배양액에 Myoinositol의 첨가는 무력정자증 환자의 인공수정시술 시 정자의 운동성과 임신율을 향상시켰다.
-
 2016년 유럽불임학회(ESHRE) P-182
다낭성난소증후군 환자의 동결융해배아 이식을 위한 효율적이고 환자친화적인 자궁내막 준비방법; letrozole을 이용한 배란유도
2016년 유럽불임학회(ESHRE) P-182
다낭성난소증후군 환자의 동결융해배아 이식을 위한 효율적이고 환자친화적인 자궁내막 준비방법; letrozole을 이용한 배란유도
